How regulatory shifts impact EMS product adoption and what companies can do to navigate the process.
The Emergency Medical Services (EMS) industry thrives on rapid response and life-saving interventions, yet the introduction of new treatments, devices, and protocols is often slowed by regulatory barriers. While these policies exist to maintain safety and consistency, they can also delay or prevent the adoption of innovations that could improve patient outcomes.
Policy change is often the missing link between technological advancement and real-world implementation. A treatment may be FDA-approved and widely used in hospitals, but unless EMS regulations and protocols allow it, frontline providers can’t carry or administer it. Recent years have shown that regulatory reform can open doors to better patient care, from expanding medication access to redefining EMS scope of practice.
Through case studies of successful EMS policy updates and strategies for navigating the regulatory landscape, this article explores how companies, agencies, and policymakers can work together to drive EMS innovation.
The Impact of Regulatory Shifts on EMS Product Adoption
Unlike hospitals, where medical staff and administrators decide which new treatments to implement, EMS adoption is determined by external governing bodies at the local, state, and national levels. These include state EMS offices, which oversee medical protocols and licensing, and medical directors, who determine whether treatments align with best practices. Additionally, state and federal legislators influence EMS through funding decisions and regulatory frameworks.
Without explicit approval at these levels, EMS providers may not be able to carry or administer a product, even if it is proven safe and effective. Policy updates, therefore, become the gateways to innovation, allowing new medications, devices, and protocols to become standard practice in the field.
Recent policy changes surrounding epinephrine administration, naloxone expansion, and whole blood transfusion provide clear examples of how regulatory reform can transform prehospital care and improve patient outcomes.
Case Studies: When Policy Opened the Door to EMS Innovation
Expanding Epinephrine Access for Anaphylaxis Treatment
For years, EMTs were restricted from administering epinephrine, the first-line treatment for severe allergic reactions. Many states only allowed paramedics to administer it via syringe, leaving Basic Life Support (BLS) providers unable to intervene, even when they arrived on the scene first.
Regulatory changes gradually expanded epinephrine access, first through auto-injectors and later through vial-and-syringe kits. This shift allowed EMTs to administer life-saving treatment immediately, reducing the time to intervention in anaphylactic emergencies.
These changes also demonstrated how cost considerations influence policy. Initially, auto-injectors were the only approved option for EMTs, but their high cost led states to revise policies again, allowing agencies to use less expensive epinephrine vials with syringes.
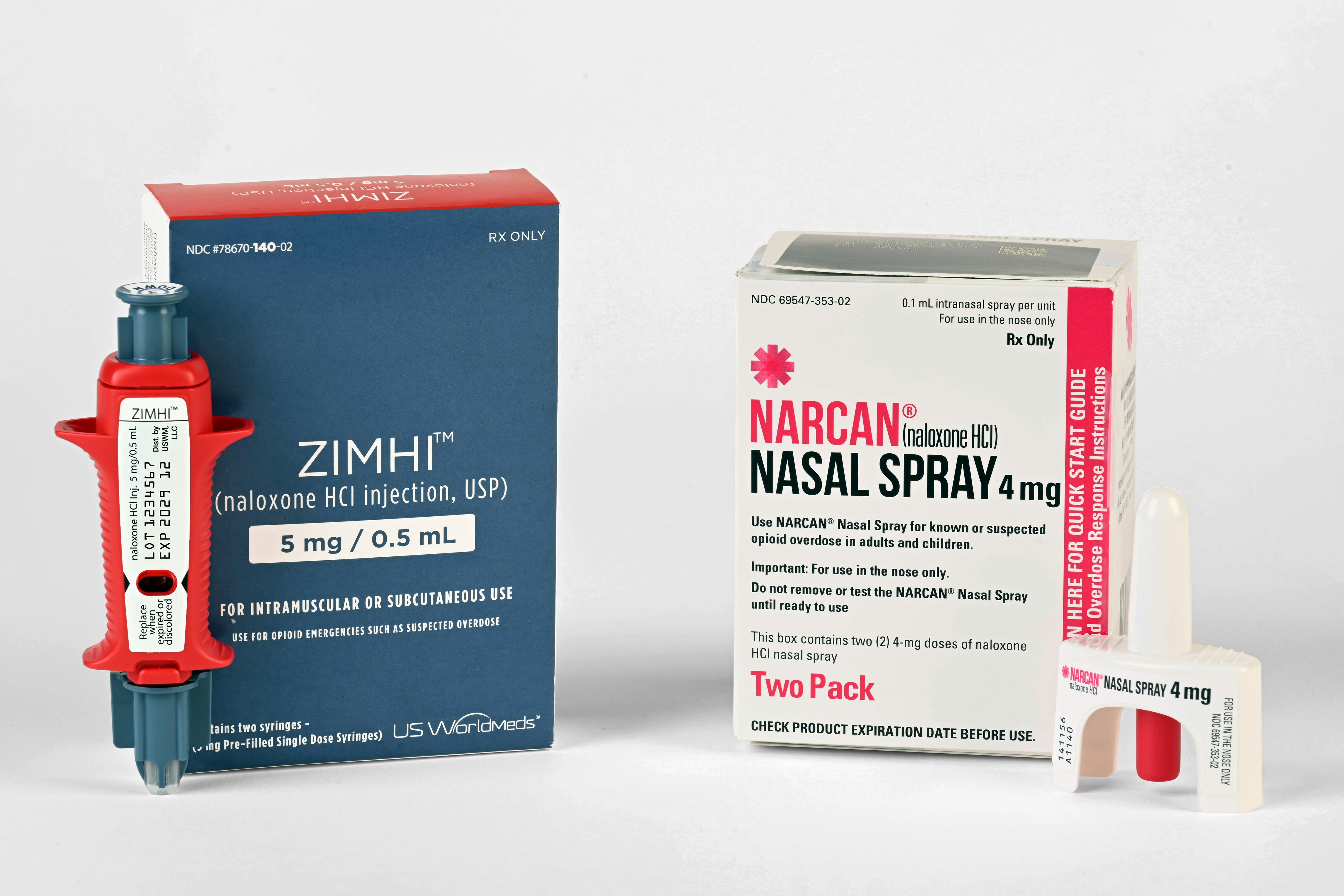
The Naloxone (Narcan) Expansion: From ALS to BLS Providers
Opioid overdoses remain one of the most time-sensitive emergencies EMS providers face. In the past, only paramedics were authorized to administer naloxone (Narcan), despite its ease of use and proven effectiveness in reversing overdoses.
As opioid deaths surged, research demonstrated that expanding naloxone access to EMTs and law enforcement personnel could save thousands of lives. Many states responded by changing policies to allow BLS providers to administer naloxone, significantly increasing the number of first responders equipped to reverse overdoses.
This regulatory shift not only improved patient outcomes but also reduced the burden on ALS units, ensuring that advanced-level providers could focus on critical cases.
Whole Blood in Prehospital Trauma Care
For decades, EMS trauma protocols relied on IV fluids, despite research showing that whole blood transfusions drastically improve survival rates in hemorrhagic shock. Regulatory barriers, however, prevented EMS from administering blood products in most states.
That began to change when pilot programs in Texas and North Carolina demonstrated that prehospital blood administration increased survival rates in trauma patients. These studies led to policy shifts allowing paramedics to carry and administer whole blood in select EMS systems, particularly in high-trauma regions like Houston, Austin, and Charlotte.
By aligning policy updates with clinical evidence, these EMS agencies were able to modernize trauma care and improve patient outcomes.
Navigating EMS Regulations to Introduce New Technology
For companies developing new medical devices, pharmaceuticals, or EMS technologies, navigating the regulatory landscape is just as important as product innovation. Even with FDA approval, a product may face significant roadblocks at the EMS level due to scope-of-practice limitations, training requirements, and budget constraints.
The key to overcoming these challenges is early engagement with EMS decision-makers. Medical directors, in particular, play a crucial role in shaping protocol changes and can provide valuable insights into potential adoption barriers. Engaging them early in the process allows companies to address clinical concerns, logistical challenges, and regulatory hurdles before they become obstacles.
Market research is another critical component of successful EMS product introduction. Conducting focus groups and provider surveys helps companies understand how a product will fit into existing EMS workflows, what training might be required, and whether frontline providers see value in its use. This research can also inform cost-benefit analyses, which are essential for securing agency buy-in and funding approval.
For some products, policy change may be necessary before adoption can occur. Companies should be prepared to work with state EMS offices, medical associations, and advocacy groups to push for regulatory updates when needed. Pilot programs can be a powerful tool in this effort, providing real-world data to support legislative discussions and protocol revisions.
Training and education also play a vital role in EMS adoption. Even when a product is approved for EMS use, agencies must feel confident that providers can integrate it effectively into patient care. Companies should invest in continuing education programs, hands-on training sessions, and scenario-based demonstrations to ensure successful implementation.
Policy Change as a Path to EMS Innovation
EMS providers need access to the best tools, medications, and technologies to improve patient outcomes, but regulatory hurdles can delay or prevent the adoption of life-saving innovations. Companies entering the EMS space must recognize that policy change is often a necessary step in the adoption process and be prepared to engage with regulators, medical directors, and advocacy groups to drive progress.
By aligning product strategy with EMS regulations, companies can ensure their innovations aren’t just available—they’re actively used to enhance patient care and improve survival rates.
Are you introducing a new product to the EMS market? TheVitals can help you navigate regulations, engage decision-makers, and develop a strategy for success. [Contact us today.]